Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 1287 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
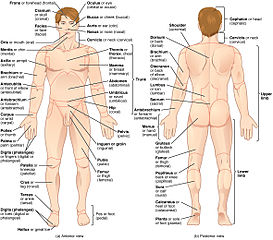
Continuing on the topic of surface anatomy, the surface of the body has been divided into anatomical regions which are used to describe locations on the body.
The number of regions varies according to different authors and even the boundaries of these regions are sometimes not clearly delineated and will vary from author to author. Still, these regions are the basis of surface anatomy.
The human body as a whole can be divided into eight basic regions:
• Head
• Neck
• Torso (itself divided into abdomen and thorax)
• Superior extremities (not to be confused with “the leg”)
• Inferior extremities (not to be confused with “the arm)
The division of thorax and abdomen is not clearly evident, as the respiratory diaphragm, which is considered the boundary between them is curved. The abdomen is divided into nine abdominal regions and four abdominal quadrants.
Original image courtesy of Connexions (http://cnx.org) [CC-BY-3.0 (http://creativecommons.org/licenses/by/3.0)], via Wikimedia Commons
- Details
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.

Philippo Verheyen
Philippo Verheyen (1648 – 1710). Flemish physician and anatomist, Philipo (Philip) Verheyen was born in the city of Verrebroek in Belgium, worked as a farmer in his early years and was probably expected to be a farmer for the rest of his life. The local Catholic parish pastor Johannes Jaspars, recognizing his intelligence, started teaching him Latin and letters with the intention of having Philip become a priest.
In 1672, he was sent to the Trinity College in Leuven where he started his studies in arts and later in theology. He continued his studies in Theology at the Collegium Sancti Spiritus (College of the Holy Spirit). During the latter part of his studies Verhayen was already wearing a priest’s collar. In 1675 Verheyen suffered an injury that lead to gangrene and eventual amputation of his left leg. This injury prevented him from taking his final vows as a priest.
Verheyen enrolled at the University of Leuven College Of Medicine where after 3 years he became a physician. Unhappy with his mostly theoretical medical knowledge Verhayen moved to Leyden to continue his studies with Frederick Ryus and others.
In 1683 Verheyen returns to Leuven where he presents his doctoral thesis which is accepted. In August 1669 elected Rector Magnificus at the University of Leyden, one of the highest honors ever bestowed on him. This is why Verheyen's statue is among the personalities honored at the town hall in Leuven, Belgium.
Verheyen was a prolific writer including several books and manuscripts. His main work “Corporis Humani Anatomiae”, a two book work, had twelve editions, some in other languages besides Latin. This book became one of the most used anatomy books until the middle of the 18th century. Interestingly, Verheyen relates his life and studies at the beginning of his book in a chapter call Compendium Vitae (CV). Only the first edition was published while Verheyen was alive.
The following excerpt of his book "Corporis Humani Anatomiae Liber Primus" reads : " ... QuintusAuricularis, quia cum minimum sit, auribus expurgandis est aptissimus" translates as"..the fifth (finger, called) Auricularis, because how small it is, is most suitable to clean the ears". Incredibly, anatomists at that time called the fifth digit "digitus auricularis".
Verheyen is credited with the creation of the eponym the “Achilles tendon” which denominates the common tendon for the gastrocnemius and soleus muscle, although at the time he called it the “Chorda Achillis”. He also described the kidneys in detail, especially the arterial “stars” found on the surface of the kidney, which are today known as the “Stars of Verheyen”.
In 2005 an article appeared on the World Wide Web with a painting showing Verhayen dissecting his own amputated leg. This initially “anonymous” oil pintingis actually a Photoshop-edited image which incorporates parts of the painting “The Anatomy Lesson of Dr. Nicolaes Tulp” by Rembrandt. This work was made by ShrestaRit Premnath. This is a conceptual artwork depicting the concept of amputation, but not an actual oil painting, as shown by the image analysis depicted at the bottom of this article.
The story of Verheyen keeping and dissecting his own leg is most probably a myth for several reasons. Verhayen was poor and did not have enough money to go to Leyden to have his leg amputated there as the myth suggests. Preservation techniques were not too good at the time and when Verheyen had his leg amputated he had yet to enter medical school and be introduced to the art of human anatomy. Granted, he had dissected animals before in the farm, but it is doubtful that this myth is true.
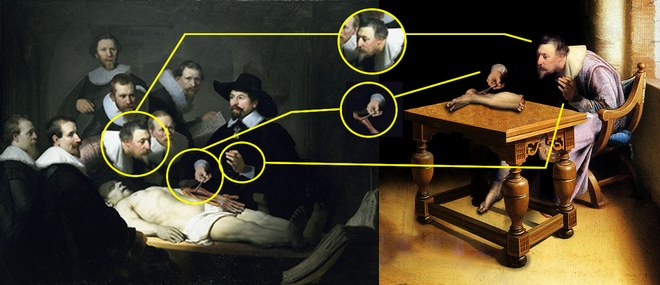
Click on the image for a larger version.
The image above shows a comparison between Rembrandt's painting “The Anatomy Lesson of Dr. Nicolaes Tulp” and an "anonymous" oil painting that appeared on the Internet circa 2005.
This oil painting include elements from Rembrandt's work. First, the head of "Verheyen" has been copied and flipped horizontally, This causes "Verheyen's" neck position to be awkward for the job of dissection. Second, the right hand holding the dissector and Achilles' tendon is Dr. Tulp's hand that has been slightly rotated, including the instrument anf the cuff. Third, the left hand is also that of Dr. Tulp, but not the cuff. If you look closely you will notice that both cuffs are different!
I have not been able to find the original painting on which these elements were added. My guess is that the left leg depicted on the table is also added. Interestingly, the table shows perspective problems.
In 2023 I had the honor of being invited by the University of Antwerp in Belgium to speak at the 2023 Vesalius Triennial Meeting in the city of Antwerp, Belgium. While there I visited Verrebroek, the city where Verheyen was born.
Personal note: I am proud to have in my library catalog a copy of the second edition of Philippo Verheyen's “Corporis Humani Anatomiae, Liber Primus”, published in 1710 in Brussels by the printer house of Fraters Serstevens. The book is signed by an Ex-Libris by "Hanolet". I have not been able to find more information on this prior owner of this book. An image of the title page is depicted in this article. Dr. Miranda
Sources
1. “Philip Verheyen (1648-1710) and his Corporis Humani Anatomiae” Suy R. Acta chir belg, 2007, 107, 343-354
2. “Achilles tendon: the 305th anniversary of the French priority on the introduction of the famous anatomical eponym” Musil, V. et al Surg Radiol Anat (2011) 33:421–427
3. "Philip Verheyen" Research and movie by digitalstories.be by Hedwige Daenens
Original image courtesy of the National Library of Medicine
- Details
This is the second most popular article on this blog!
Look at the hits counter on this article...
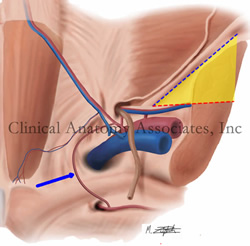
Image property of: CAA.Inc.. Artist: M. Zuptich.
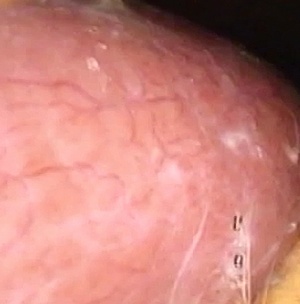
The so-called "triangle of pain" is a misnomer coined by laparoscopic hernia surgeons who observed the anatomy of the inguinofemoral region from the posterior aspect and refers to an inverted "V" shaped area which should be avoided because of the potential to damage nerves when placing staples, tacks, or sutures to anchor a mesh during a laparoscopic herniorrhaphy.
An example of a similar situation with terminology is the so-called "triangle of doom". It is also not a triangle, as it only has two boundaries. similarly, it does indicate an area where it is dangerous to place staples or sutures during laparoscopic hernia surgery.
The "triangle of pain" is an inverted "V" shaped area with its apex at the internal (deep) inguinal ring. It is bound anteriorly by the iliopubic tract / inguinal ligament and by the testicular (spermatic) vessels posteromedially. This "triangle" has no defined posterolateral boundary. although you can see it in drawings by some authors.
The reason why this area should be avoided and not place staples or sutures to anchor a hernia mesh is that there are several nerves which usually cannot be seen as they run just deep to the endoabdominopelvic fascia.These nerves can suffer damage or entrapment when performing a laparoscopic herniorrhaphy and cause pain (hence the name of the area) as well as motor and sensory disorders.
The nerves are:
• Lateral femoral cutaneous nerve: arising from the ventral rami of L2 and L3, this nerve provides sensory innervation to the anterior skin of the thigh
• Femoral nerve: arising from the ventral rami of L2, L3, and L4, this nerves provides motor and sensory innervation to the anterior compartment of the thigh as well as sensory branches to the hip joint
• Genitofemoral nerve: arising from the ventral rami of L1 and L2, this nerve divides anterior to the psoas major muscle into two branches. The genital branch of the genitofemoral nerve enters the inguinal canal and provides sensory and motor innervation to the scrotum and cremaster muscle, as well as the labia majora and mons pubis. The femoral branch of the genitofemoral nerve enters the "triangle of pain" region and passes inferior to the inguinal ligament to provide sensory cutaneous innervation to the superior aspect of the thigh.
The image shows a posterior view of the inguinal region. The "triangle of pain" is depicted in yellow. The iliopubic tract / inguinal ligament is shown by a blue dotted line while the testicular vessels boundary is shown by a red dotted line. The blue arrow points to the aberrant obturator artery (Corona Mortis).
Thanks to Steve Pearson for suggesting this term. Medical illustration by Mark J. Zuptich.
Clinical anatomy of the inguinofemoral hernias, as well as abdominal and perineal hernias are some of the lecture topics developed and delivered to the medical devices industry by Clinical Anatomy Associates, Inc. For more information Contact Us.
- Details
The noun word [porta] is Latin and means "gate" or "door". The adjectival form [portal] means “pertaining to a door”. These terms are used in anatomy and pathology to denote the entrance to an organ.
• porta hepatis: The entrance or "door" to the liver
• portal vein: The vein that enters through the porta hepatis
• portal system: A system of veins that collects the venous return from the digestive system and derives it through the portal vein into the liver
• portal hypertension: A pathological condition of higher blood pressure in the portal vein system.
- Details
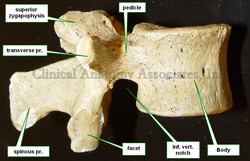
The lumbar region of the spine is composed by five lumbar vertebrae. Although sharing characteristics common to all vertebrae, a lumbar vertebra can be differentiated by the following:
• The vertebral body is large, tall, and when viewed from superior, the vertebral body has a longer transverse diameter and a shorter anteroposterior diameter. Most anatomists describe the vertebral body as being “kidney-shaped”. The massiveness of the vertebral body is due to the larger weight that each consecutive vertebra has to bear in the lumbar region. Because of this, lumbar vertebrae have larger anular epiphyses, and the vertebral body is hourglass-shaped with a “waist”. As with other vertebrae, the body of a lumbar vertebra has vertebral endplates, nutritional foramina, and in its posterior aspect they present with basivertebral foramina.
• The pedicles in the lumbar vertebrae are larger, course in a mostly anteroposterior direction, and have a oval cross-section where the superoinferior diameter is longer and the transverse diameter is shorter. This is important for transpedicular procedures for vertebroplasty or kyphoplasty.
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore
• The transverse processes are also larger than other vertebrae. Of interest are the facts that the transverse process of the third lumbar vertebra is the longest of all lumbar vertebrae and that the transverse process of the fifth lumbar vertebra courses superolaterally at an angle of almost 45 degrees because of the presence of the strong iliolumbar ligament. The lumbar transverse processes have a small tubercle called the mammillary process.
• The lumbar spinous processes are large and have a square shape.
Again, because of the larger weight bearing capacity of the lumbar vertebrae, they have strong ligaments and their zygapophyseal joints and articular facets tend to be oriented with their surfaces in a transverse plane. This has two consequences: The rotational mobility of the whole lumbovertebral region is limited and they tend not to have anteroposterior displacement.
Image property of CAA.Inc. Photographer: D.M. Klein.
- Details
UPDATED: The term [ischemia] arises from the Greek word [ισχαιμία], meaning "to slow down the flow of blood". The root portion arises from the Greek [σφίγγω] meaning "to constrict" or "to stop". The uffix is [-emia] from the Greek [αίμα] (ema) meaning blood. Another potential origin is the Greek word [ischanein], meaning " to keep at bay" or 'to hold in check". It was Rudolf Virchow (1821-1902) who first used the term [ischemia] to denote a local reduction in the flow of blood.
Today the term ischemia means "localized reduction in the flow of blood to an organ or region of an organ". Ischemia occurs when there is a stenosis or stricture of an artery.
Note: The links to Google Translate include an icon that will allow you to hear the Greek or Latin pronunciation of the word.