
Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 786 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
- Written by: Efrain A. Miranda, Ph.D.
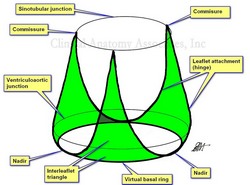
Interleaflet triangles of the aortic valve by MTD.
Click for a larger image.
The interleaflet triangles (ILTs) are three triangular regions found in the ventricular aspect of the aortic root. They are bound inferiorly by the virtual basal ring (VBR), laterally by the attachment of the leaflets (the hinge) to the aorta and left ventricular wall (muscular and fibrous), and superiorly by the commissures (site of attachment and meeting of adjacent leaflets) which are usually located at the sinotubular junction, also known as the sinotubular ridge.
A review of the literature on the topic shows that although many speak of these ILTs, not many authors have clearly defined their boundaries. In fact, some only reserve the term ILT to the triangular region distal to the ventriculoaortic boundary. The description used in this article includes the ventricular wall found between the VBR and the ventriculoaortic junction as well as fibrous components found between these two boundaries. Based on this description, we have developed an image of the ILTs that, to our knowledge is not found in literature. (see accompanying images).
The virtual basal ring is a circular virtual line formed by the nadirs of the three aortic leaflets (cusps). The attachment of the three leaflets create a three-pronged coronet that is useful in defining the interleaflet triangles (see image)
The superior boundary of the ILTs is formed by three commissures, the points where the leaflets meet each other at the sinotubular junction. There are two posterior commissures, right and left. The right-posterior commissure is found between the noncoronary and the left coronary sinuses (of Valsalva). An important point about this commissure is that it is situated above the midpoint of the septal (anterior) leaflet of the mitral valve. The left-posterior commissure is found between the left and the right coronary sinuses. The anterior commissure is located between the right and the noncoronary sinus close to the membranous interventricular septum.
Based on the above description, there are three interleaflet triangles:
a. Right (posterior), left (posterior), and anterior. The right posterior ILT is located between the noncoronary and the left coronary sinuses, and just as the commissure at its apex, is located at the midpoint of the septal (anterior) leaflet of the mitral valve. Also, the superior aspect of this ILT is related to the transverse pericardial sinus.
b. The left posterior ILT is located between the right and the left coronary sinuses, and is lies immediately behind the right ventricular outlet.
c. The anterior ILT is found between the right and the noncoronary sinuses. It is related to the membranous septum and the right fibrous trigone, forming part of the central fibrous body (skeleton) of the heart. This ILT is a good anatomical landmark to the location of the bundle of His and the left bundle branch, both components of the conduction system of the heart. These structures can be compressed during the implantation of an aortic or mitral valve, causing transitory or permanent cardiac conduction problems.
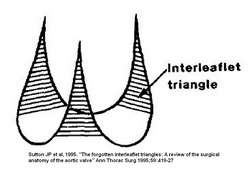
Interleaflet triangles of the aortic valve by Sutton.
Click for a larger image.
The ILTs are important in the normal physiology and hemodynamics of the aortic valve. A small ILT will affect the diameter of the valve and the movement of the leaflets, causing stenosis. This is the case in bicuspid aortic valves where the fusion of two of the leaflets leads to the reduction in size of the ILT normally found between these two fused leaflets.
Since they are located within the functional portion of the left ventricle, the ILTs are subject to the pressures of the ventricle and can be areas that develop aneurysms.
Because of their importance in the hemodynamics of the aortic valve, new procedures and medical devices that reshape the ILTs are being developed. This is specially important in the case of a bicuspid aortic valve, where the interleaflet triangles may be abnormal.
Further to the images that are depicted in this article, the lower image is the classic image of the interleaflet triangles by Sutton (1995). As you can see, the base of the triangles is shown straight with no clear boundary, and it seems as though they are related to the ventriculoaortic junction. The nadirs are not used as a point of reference. The upper image (developed by us and based on Sutton's original sketch) clearly shows the extent of the ILTs as well as their relation to the three landmarks that define the aortic root: The virtual basal ring, the ventriculoaortic junction, and the sinotubular junction.
NOTE: The pulmonary valve also has interleaflet triangles, with a somewhat similar description, but since they are under low pressure they do not develop or are cause of pathology as the ILTs of the aortic valve.
Sources:
1. The Anatomy of the Aortic Root: Loukas, M et al. Clinical Anatomy 27:748–756 (2014)
2. “Extracardiac aneurysm of the interleaflet triangle above the aortic-mitral curtain due to infective endocarditis of the bicuspid aortic valve.” Hori D, et al. Gen Thorac Cardiovasc Surg. 2008 Aug;56(8):424-6
3. “Anatomy of the aortic root: implications for valve-sparing surgery” Efstratios I. Charitos, HS. Ann Cardiothorac Surg 2013;2(1):53-56
4. “The Forgotten Interleaflet Triangles: A Review of the Surgical Anatomy of the Aortic Valve” Sutton JP, et al Ann Thorac Surg 1995;59:419-27
5.” The aortic interleaflet triangles annuloplasty: a multidisciplinary appraisal” Mangini, A., et al. European Journal of Cardio-Thoracic Surgery, Vol. 40:4, 2011, 851-857
6. “Structure and Anatomy of the Aortic Root” Ho, SH., Eur J Electrocar 2009 10; i3-i10
7. “In vitro study of the aortic interleaflet triangle reshaping” Vismara, R Journal of Biomechanics; 47:2; 2014. 329-33
- Details
- Written by: Efrain A. Miranda, Ph.D.
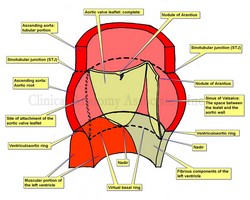
Aortic root and aortic valve.
Click for a larger image.
This article is a continuation of: The aortic root and the aortic valve (1)
The aortic valve is formed by three semilunar leaflets which are very thin as to be almost transparent. The attachment of the leaflets is complex, as part of them attaches to ventricular wall, part attaches to the sinusal arterial wall, and even part of them attaches to the membranous interventricular septum and other fibrous structures. Loukas et al state that at “least one third of the circumference of the aortic root is supported by fibrous tissue rather than ventricular musculature”
Each of the three aortic leaflets has a semilunar attachment and shape (hence the term “semilunar valve” used for both the aortic and pulmonary valve, as they have similar shape). The attachment of these three leaflets create a continuous line where the highest points are the three locations where the leaflets attach at the STJ, and the three lower points or “nadirs” form an edge shaped like a three-pronged “coronet”. This coronet is called by many the “anatomical anulus” of the aortic valve, as this is where the fibrous skeleton of the heart forms the “hinges” of the aortic valve.
The leaflets of the aortic valve (as well as those in the pulmonary valve) have a tissue excrescence that can become quite hard at the point where the three leaflets touch on each heartbeat. These are the nodules of Arantius, named after Giulio Cesare Aranzio (1530 – 1589). As a side note, the nodules of the pulmonary valve have a different name. Distally, the aortic leaflets may present a very thin extension that may be cribriform (not shown in the sketch). These are called the lunulae (singular: lunula) as they look like a sliver of moon.
The second component of the base of the aortic root is a ring defined by the lowest portion of each leaflet, the nadir. This ring is called the “virtual basal ring”, is found within the left ventricle and is used as a surgical reference for aortic valve replacement implants.
The three leaflets are found within three dilations of the aortic root, each one called a “sinus of Valsalva”, which extend between the virtual basal ring inferiorly and the STJ superiorly. The presence of the sinuses of Valsalva permits “fluttering” of the open aortic leaflets in ventricular systole. This fluttering of the leaflets allows blood to flow into the sinuses and into the coronary arteries during ventricular systole.
Aortic valve may present with different number of leaflets, as in the case of a bicuspid aortic valve.
The shape of the attachment of the leaflets create two distinct situations:
First, there is a portion of the ventricle related to the leaflets where the ventricle acts as an artery, the aorta. These areas are found inside the sinuses of Valsalva.
Second, there are triangular areas of the aortic root (the interleaflet triangles) where the aortic wall is within the left ventricle and submitted to the pressures and hemodynamics of the left ventricle. These interleaflet triangles have been involved in aneurysms. For simplicity, these interleaflet triangles are not shown in the sketch and are the subject of a separate article in this website.
Note: The image depicts only one complete aortic leaflet. The other one has been transected to show the sinus of Valsalva and the third has been removed to show the attachment or "hinge" of the leaflet. For an anatomical image of the aortic valve click here.
Sources:
1. The Anatomy of the Aortic Root: Loukas, M et al. Clinical Anatomy 27:748–756 (2014)
2. “Extracardiac aneurysm of the interleaflet triangle above the aortic-mitral curtain due to infective endocarditis of the bicuspid aortic valve.” Hori D, et al. Gen Thorac Cardiovasc Surg. 2008 Aug;56(8):424-6
3. “Anatomy of the aortic root: implications for valve-sparing surgery” Efstratios I. Charitos, HS. Ann Cardiothorac Surg 2013;2(1):53-56
4. “The Forgotten Interleaflet Triangles: A Review of the Surgical Anatomy of the Aortic Valve” Sutton JP, et al Ann Thorac Surg 1995;59:419-27
Image property of: CAA, Inc. Artist: Dr. Miranda
- Details
- Written by: Efrain A. Miranda, Ph.D.

Aortic root and aortic valve.
Click for a larger image.
The term “aortic valve” refers to the three leaflets (or cusps) components that allow passage of blood from the left ventricle to the ascending aorta during ventricular systole, while at the same time preventing regurgitation or reflux of blood back into the ventricle during ventricular diastole. In reality, the “valve” is only a component of a larger structure called the “aortic root”. This article will describe the components of the aortic root and the aortic valve.
The ascending aorta presents with two distinct segments. The proximal segment is a dilated portion called the aortic root. The distal portion is known as the tubular portion of the ascending aorta. The boundary between these two portions is the [sinotubular junction (STJ). Some authors will recognize as the ascending aorta only the tubular portion.
The aortic root is that portion of the ventricular outflow tract and proximal aorta that supports the leaflets of the aortic valve. It is a functioning unit with relations both to the to the aorta and to the left ventricle, and it is here where in most cases we find the ostia of the right and left coronary arteries.
The aortic root is composed of the three dilated sinuses of Valsalva, two of which give origin to the coronary arteries (right and left), three leaflets (or cusps), and the interleaflet triangles. While the distal boundary of the aortic root is clearly defined (the STJ), the proximal boundary is not as clear and is difficult to define. The STJ is defined by the apices of the three aortic leaflets as well as a clear line that appears as the aorta passes from the dilations of the sinuses of Valsalva to the well-defined tubular portion of the ascending aorta.
This proximal boundary is defined clinically by two circular regions: the ventriculoaortic ring distally and the virtual basal ring proximally.
The ventriculoaortic ring is a circular region formed by the left ventriculoaortic junction (the point where the aorta anchors on the left ventricle), and fibrous tissue of both the “cardiac skeleton” and the membranous interventricular septum. It is also called the “surgical anulus”. This is the area where a surgeon will anchor an aortic replacement valve.
Continued here: The Aortic Root and the Aortic Valve (2)
Note: The image depicts only one complete aortic leaflet. The other one has been transected to show the sinus of Valsalva and the third has been removed to show the attachment or "hinge" of the leaflet. For an anatomical image of the aortic valve click here.
Sources:
1. The Anatomy of the Aortic Root: Loukas, M et al. Clinical Anatomy 27:748–756 (2014)
2. “Extracardiac aneurysm of the interleaflet triangle above the aortic-mitral curtain due to infective endocarditis of the bicuspid aortic valve.” Hori D, et al. Gen Thorac Cardiovasc Surg. 2008 Aug;56(8):424-6
3. “Anatomy of the aortic root: implications for valve-sparing surgery” Efstratios I. Charitos, HS. Ann Cardiothorac Surg 2013;2(1):53-56
4. “The Forgotten Interleaflet Triangles: A Review of the Surgical Anatomy of the Aortic Valve” Sutton JP, et al Ann Thorac Surg 1995;59:419-27
Image property of: CAA, Inc. Artist: Dr. Miranda
- Details
- Written by: Efrain A. Miranda, Ph.D.
Andreas Vesalius Bruxellensis (1515-1564) is considered to be the father of modern anatomy, remembered because an illustrious life and by his book “De Humani Corporis Fabrica, Libri Septem” published first in 1543. Scores of books, translations, articles, and analyzes of his work have been published in the over 500 years since his birth.
With such an incredible pedigree we would expect his name to be attached to more than a few anatomical structures, many of which were first described in his opus magnus, the “Fabrica”, I wonder why this is not so. It is true that modern anatomy is trying to move from eponyms to more descriptive anatomical terms. Still, there are many that will not go away, as is the famous ligament of Treitz, or the sphincter or Oddi.
Today there is only one recorded eponym for Andreas Vesalius, the os vesalianum, a rare accessory bone in the foot located proximally to the base of the fifth metatarsal. It is usually asymptomatic, but in rare cases it can cause pain. It is formed by the failed fusion of the secondary ossification center of the fifth metatarsal.
Reviewing history, I was able to find other references to Andreas Vesalius eponyms or potential eponyms, now in disuse or misnamed:
- Suspensory ligaments of the mammary gland. Although first described by Vesalius in the Fabrica, these structures are named after Sir Astley Paston Cooper (1768 -1841), almost 300 years after being described by the great anatomist, who called them a “fleshy membrane” that stretched between the pectoral fascia and the skin.
- The vermiform appendix. Although called by many just “the appendix”, this structure is mentioned, but not named, by Jacobo Berengario da Carpi in 1524. It was Andreas Vesalius who first described it as an appendix, suggested it looked like a worm (Lat: vermis) calling it the “vermiform appendix”.
- The ligamentum suspensorium Vesalii or crural arch. First described by Giovanni Baptista Morgagni (1682-1771), it was named in honor of Vesalius by Dr. Laurentii (Lorenz) Heisters in his “Compendium Anatomicum” published in 1756. Other authors point to Gabrielle Fallopius as the first to describe this structure in 1561, although he did publish later than Vesalius (1543). Although named after Vesalius, it was later named after Francois Poupart who described it in 1695. You probably know this structure as the inguinal ligament.
- The ligamentum teres femoris. The round ligament of the femur was also first described by Vesalius in 1543.
NOTE: If you have other structures that have been named after Vesalius, please let me know by clicking here
Sources:
1. “A Rare Cause of Foot Pain with Golf Swing. Symptomatic Os Vesalianum Pedis—A Case Report” Petrera, M et al. Sports Health. 2013 Jul; 5(4): 357–359.
2. “Andreas Vesalius’ 500th Anniversary: First Description of the Mammary Suspensory Ligaments” Brinkman RJ, Hage, JJ. World J Surg (2016) 40:2144–2148
3. “Compendium Anatomicum” Heisters, L. 1756 (German)
4. “Anatomy: An Encyclopedic Reference to the Language of Anatomy and Neuroanatomy. It Provides the Fascinating Origin of Terms and Biographies of Anatomists/Physicians Who Originated Them” Bergman, RA, Afifi, AK 2016
- Details
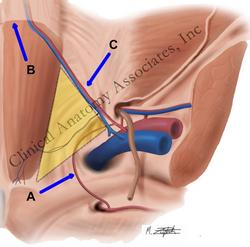
Hesselbach's triangle.
Click for a larger image.
UPDATED: From the Greek [ep(i)] meaning "outer, above, or upon", and the Greek suffix [o-nym] meaning "name". The word [eponym] refers to a person's name becoming attached to an anatomical location or surgical procedure. For centuries it has been the custom to honor or remember someone by attaching their name to a structure, location, procedure, or maneuver.
This has changed as anatomists tend now to give locations and structures descriptive terms. An example of this would be the "Ampulla of Vater" named after the German anatomist Abraham Vater (1684-1751) described today in anatomical texts as the "hepatopancreatic ampulla". The controversy on using eponyms or not goes on...
There are many eponymical terms in the medical arena; following are some of them, click on the links for additional information:
• Hesselbach’s triangle: Named after Franz Kaspar Hesselbach (1759-1816) (see yellow insert in superior image)
• Spigelian line (linea semilunaris): Site for an Spigelian hernia, named after Adrian Van Der Spigelius (1578-1625) (see blue arrow in inferior image)
• Fallopian tube: Named after Gabrielle Fallopius (1523-1563)
• Cooper's pectineal ligament. Named after Sir Astley Paston Cooper (1768-1841)
• Hartmann's procedure: A two-stage colon resection and anastomosis. Named after Prof. Henri Hartmann (1860-1952), a French surgeon.
• Heimlich's maneuver: Named after Dr. Henry J. Heimlich (1920 - 2016)
• Ligament of Treitz: Named after Václav Treitz (1819 - 1872), a Czech pathologist.
• Sphincter of Oddi. Named after Ruggero Oddi (1864 - 1913), an Italian anatomist.
If you want to see a listing of the eponyms in this website, click here.
Here is an article on "The lost influence of Andreas Vesalius on eponymic anatomy".
Here is an interesting article on eponyms by Ilana Yurkiewicz published on 11/15/2012 in Scientific American: "Modern medical terms are still named after Nazi doctors. Can we change it?". It is interesting and thougthful reading.
PERSONAL NOTE: Many anatomists today are actively trying to eliminate eponyms from anatomical, medical, and surgical books. For me, this eliminates the interest of learning about the people who either first described these structures or procedures, which is one of the objectives of this website. I wonder (and this is a tongue-in-cheek comment) if the reason for this desire to eliminate eponyms is because there are so many attached to anatomical structures that there is no place for their own names! When history has forgotten about the original eponyms maybe we will see new ones with the names of modern anatomists! I do not worry, my name is attached to the "Ligaments of Miranda"... don't ask! Dr. Miranda
Superior image property of: CAA.Inc.. Artist: M. Zuptich.
Inferior image property of :CAA.Inc.. Artist:D.M. Klein
- Details
UPDATED: The ascending aorta is the first and most proximal portion of the aorta. About 5 cm. in length and 3 cm. in diameter at its origin, its proximal end begins at the superior aspect of the outflow tract of of the left ventricle, at the ventriculoaortic junction.
The ascending aorta ends superiorly at an imaginary horizontal plane (blue dotted line) that passes through the sternal angle (of Louis), continuing distally with the aortic arch. This is an important anatomical landmark, as many surgeons use as the superior border of the ascending aorta an oblique plane that passes proximal to the brachiocephalic trunk (yellow dotted line). Although this landmark could be useful in surgery, it is not anatomically correct.
Since the sternal angle (of Louis) also indicates the superior border of the pericardial sac, it can be said that the ascending aorta is completely intrapericardial, and in surgery the pericardial sac should be the anatomical landmark used to separate the ascending aorta from the aortic arch.
From its point of origin at the ventriculoaortic junction, the aorta presents with a dilated region where the aortic valve is located. The aortic valve is one of the two semilunar valves of the heart, and the dilation of this region is caused by the presence of the sinuses of Valsalva. This dilated bulbous segment is known as the aortic root.
The dilated, sinus portion, or aortic root segment of the ascending aorta continues superiorly with the tubular portion of the ascending aorta. The area of transition between these two components is marked by a sharp crease known as the sinotubular junction (STJ). The dilation of the aortic root is caused by the presence of the sinuses of Valsalva, named after Antonio Maria Valsalva (1666 - 1723).
The tubular portion of the ascending aorta ascends with an inclination anteriorly and to the right. The ascending aorta presents with a slight anterior bulge causing the transverse section of this aortic segment to be slightly oval.
Only two arteries arise from the ascending aorta, both usually at the aortic root segment, just inferior to the STJ. These are the right coronary artery and the left coronary artery. There are anatomical variations where only one, or up to five different coronary arteries have been described.
At its origin, the aorta presents with semilunar folds of the serous surface of the pericardium. Also known as the ascending aortic folds, or Rindfleisch's folds, these are eponymically named after Georg Eduard Von Rindfleisch (1836 – 1908), a German pathologist and histologist of Bavarian nobility ancestry.
Image property of: CAA.Inc.. Artist: Dr. E. Miranda




