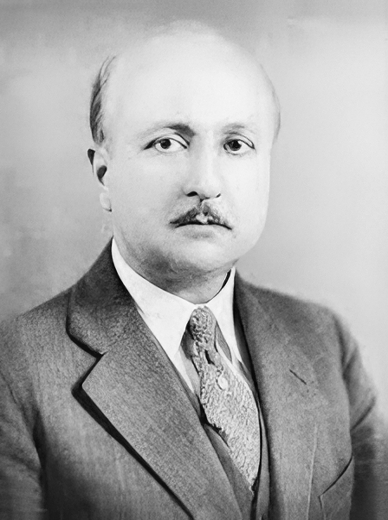Medical Terminology Daily (MTD) is a blog sponsored by Clinical Anatomy Associates, Inc. as a service to the medical community. We post anatomical, medical or surgical terms, their meaning and usage, as well as biographical notes on anatomists, surgeons, and researchers through the ages. Be warned that some of the images used depict human anatomical specimens.
You are welcome to submit questions and suggestions using our "Contact Us" form. The information on this blog follows the terms on our "Privacy and Security Statement" and cannot be construed as medical guidance or instructions for treatment.
We have 160 guests online

Marcia Crocker Noyes
(1869 – 1946)
Further to my comment on old books and research that started with an interesting bookplate (Ex-Libris). I continued my research and found that the person in charge of the Osler library bookplate was a fascinating individual that today maybe a ghost in the MedChi library and building in Baltimore... This is certainly an article that can be called "A Moment in History"
Marcia Crocker Noyes was the librarian at The Maryland State Medical Society from 1896 to 1946 and was a founding member of the Medical Library Association.[1][2][3]
Sir William Osler, MD. a famous Johns Hopkins surgeon was a noted bibliophile and had a large personal collection of books on various topics. When he became the President of MedChi in 1896, he was dismayed at the condition of the library and knew that with the right person and some stewardship, it could become a significant collection. Sir William asked his friend, Dr. Bernard Steiner, a physician and President of the Enoch Pratt Free Library in Baltimore for suggestions of a librarian, and Dr. Steiner recommended Marcia Crocker Noyes. A native of New York, and a graduate of Hunter College, Marcia had moved to Baltimore for a lengthy visit with her sister, and took a “temporary” position at the Pratt Library, which turned into three years. Although she had no medical experience or background, she was enthusiastic, and most importantly, she was willing to move into the apartment provided for the librarian, who needed to be available 24 hours a day.
The image in this article is Ms. Noyes on her first year on the job. Marcia developed a book classification system for medical books, based on the Index Medicus, and called it the Classification for Medical Literature. The system uses the alphabet with capital letters for the major divisions of medicine and lower-case ones for the sub-sections. The system was used for many years, but it's now dated and the Faculty's original shelving scheme was never changed. The card catalogs still reflect her classification and many of the cards are written in Marcia's back-slanting handwriting.
Marcia knew enough to ask the Faculty's members about medical questions, terminology and literature. She gradually won over the predominantly male membership and they became her greatest allies; Sir William at the start, and then for nearly 40 years, Dr. John Ruhräh, a wealthy pediatrician with no immediate family of his own. She made a point of attending almost every Faculty function, and in 1904, under guidelines from the American Medical Association, Marcia was made the Faculty Secretary. For much of her first 10 years, she was the Faculty's only full-time employee, only being assisted by Mr. Caution, the Faculty's janitor. Later in life Marcia would say that she hired him because of his name!
Within ten years, the library had outgrown its space, and plans, spearheaded by Marcia and Sir William before his move to Oxford, were made to build a headquarters building, mainly to house the library's growing collection of medical books and journals.
Marcia was instrumental in the design and building of the new headquarters. She travelled to Philadelphia, New York and Boston to look at their medical society buildings, and eventually, the Philadelphia architectural firm, Ellicott & Emmart was selected to design and build the new Faculty building. Every detail of the building held her imprimatur, from the graceful staircase, to the light-filled reading room, and all of the myriad details of the millwork, marble tesserae, and most of all, the four-story cast iron stacks. She was on-site, climbing up unfinished staircases, checking out the progress of the building, which was built in less than one year at a cost of $90,000.
Among the features of the new building was a fourth-floor apartment for her. She referred to it as the "first penthouse in Baltimore" and it had a garden and rooftop terrace. The library collection eventually grew to more than 65,000 volumes from medical and specialty societies around the world. Journals were traded back and forth, and physicians eagerly anticipated the arrival of each new issue. At the same time, Marcia was involved in the Medical Library Association as one of eight founding members. The MLA promotes medical libraries and the exchange of information. One of the earliest mandates of the MLA was the Exchange, a distribution and trade service for those who had duplicates or little-used books in their collections. Initially, the Exchange was run out of the Philadelphia medical society, but in 1900 it was moved to Baltimore and Marcia oversaw it. Several hundred periodicals and journals were received and sent each month, a huge amount of work for a tiny staff. In 1904, the Faculty had run out of room to manage the Exchange, so it was moved to the Medical Society of the Kings County (Brooklyn). But without Marcia's excellent administrative skills, it floundered and in 1908, the MLA asked Marcia to take charge once again.
In 1909, when the new Faculty building opened, there was enough room to run the Exchange and with the help of MLA Treasurer, noted bibliophile and close friend, Dr. John Ruhräh, it once again became successful. Additionally, Marcia and Dr. Ruhräh combined forces to revive the MLA's bulletin, which had all but ceased publication in 1908, taking the Exchange with it. This duo maintained editorial control from 1911 until 1926. In 1934, around the time of Dr. Ruhräh's death, Marcia became the first “unmedicated” professional to head the MLA. During her tenure, the MLA incorporated, the first seal was adopted, and the annual meeting was held in Baltimore. Marcia wanted to write the history of the MLA once she retired from full-time work at the Faculty, but her health was beginning to fail. She had back problems and had suffered a serious burn on her shoulder as a young woman, possibly from her time running a summer camp, Camp Seyon, for young ladies in the Adirondack Mountains. In 1946, a celebration was planned to honor Marcia's 50 years at the Faculty. But she was adamant that the physicians wait until November, the actual date of her 50 years. However, they knew she was gravely ill, and might not make it until then, so a huge party was held in April. More than 250 physicians attended the celebration, but the ones she was closest to in the early years, were long gone. She was presented with a suitcase, a sum of money to use for travelling, and her favorite painting of Dr. John Philip Smith, a founder of the Medical College in Winchester, Virginia. It was painted by Edward Caledon Smith, a Virginia painter who had been a student of the painter Thomas Sully.[4] She adored this painting and vowed, jokingly, to take it with her wherever she went.
The painting was not to stay with her for very long, for she died in November 1946, and left it to the Faculty in her will. Her funeral was held in the Faculty's Osler Hall, named for her dear friend. More than 60 physicians served as her pallbearers, and she was buried at Baltimore's Green Mount Cemetery. In 1948, the MLA decided to establish an award in the name of Marcia Crocker Noyes. It was for outstanding achievement in medical library field and was to be awarded every two years, or when a truly worthy candidate was submitted. In 2014, the Faculty began giving a bouquet of flowers to the winner of the award in Marcia's name, and in honor of her work. Much evidence exists for this tradition, as we know that the physicians, especially Drs. Osler and Ruhräh, frequently gave her bouquets of flowers. Marcia also cultivated flower gardens at the Faculty and decorated the rooms with her work.
Today, the MedChi building is open for tours and if the rumors are to be believed Ms. Marcia Crocker Noyes is still at work in her beloved library as the "resident ghost" [1][5]
NOTE: This article has been modified from the original Wikipedia article on Marcia Crocker Noyes. The article itself is well-written with interesting images of the subject. I would encourage you to visit it. The second insert is from book 00736 in my personal library and shows in pencil, the incredibly small handwriting of Marsha C. Noyes.
Sources:
1. "Marcia, Marcia, Marcia" MedChi Archives blog.
2. "Marcia C. Noyes, Medical Librarian" (PDF). Bulletin of the Medical Library Association. 35 (1): 108–109. 1947. PMC 194645
3. Smith, Bernie Todd (1974). "Marcia Crocker Noyes, Medical Librarian: The Shaping of a Career" (PDF). Bulletin of the Medical Library Association. 62 (3): 314–324. PMC 198800Freely accessible. PMID 4619344.
4. Edward Caledon BRUCE (1825-1901)"
5. Behind the scenes tour MedChiBuilding
"Clinical Anatomy Associates, Inc., and the contributors of "Medical Terminology Daily" wish to thank all individuals who donate their bodies and tissues for the advancement of education and research”.
Click here for more information
- Details
- Written by: Efrain A. Miranda, Ph.D.
- Hits: 11416
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.

Sunao Tawara, MD
UPDATED: Sunao Tawara, M.D. (1873 - 1952) Sunao Tawara was born in the prefecture of Ooita, Kyushu, Japan. Adopted by an uncle (and physician), Tawara studied English and German, and went on to the University of Tokyo medical school, where he graduated an MD in 1901.
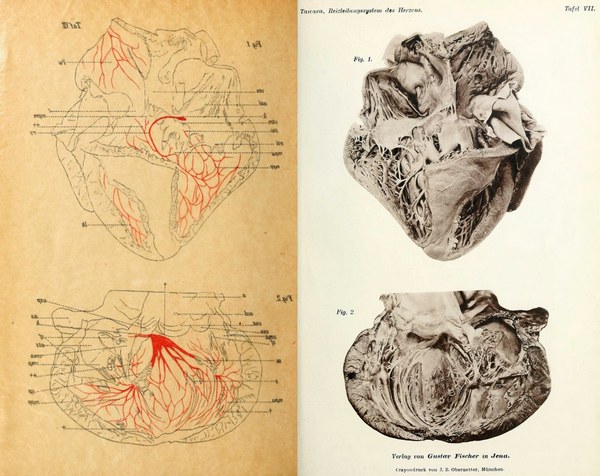
In 1903 he traveled to Marburg, Germany, where he started working under the supervision of Dr. Karl Albert Ludwig Aschoff (1866-1942), a noted pathologist. Tawara’s work led him to the discovery of what today we call the "atrioventricular node” (AV node) and the connections of the AV node and the Bundle of His by discovering the right and left bundle branches. His work with Aschoff led to the eponym of “node of Aschoff-Tawara” for the AV node. Tawara’s work also led to the understanding of the function of the Purkinje fibers. Tawara gave the entire system the name “Reitzleitungssytem” or the “conduction system” of the heart.
In 1906 Dr. Tawara published his discoveries in a German-language article entitled “The Conduction System of the Mammalian Heart — An Anatomicopathological Study on the Atrioventricular Bundle and the Purkinje Fibers”. The same year he returned to Japan and in 1908 became Professor of Pathology at the University of Kyushu until his retirement in 1933.
Not enough honors have been given to Dr. Tawara as the discoverer of some of the main components of the conduction system of the heart, such as the atrioventricular node, the left and right bundle brunches, and establishing the connection between the Bundle of His and the Purkinje fibers. William Einthoven himself cited Tawara's work as the basis to interpret an electrocardiogram.
Sunao Tawara was the sole discoverer of the AV node. Dr. Aschoff was his academic supervisor and mentor. When Tawara published his monograph, Aschoff wrote the foreword for it. At no time did he claim co-authorship of Tawara's work. The eponym "Aschoff-Tawara" node for the atrioventricular node was accepted to recognize Aschoff's support to Tawara's work.
Tawara's original monograph in German is available at archive.org. For the monograph, click here.
Sources:
1. "Sunao Tawara" Suma, K. Clin Cardiol (1991) 14; 442-443
2. "Sunao Tawara, A Cardiac Pathophysiologist" Loukas, M. et al Clinical Anatomy 21:2–4 (2008)
3. "Sunao Tawara: A Father of Modern Cardiology" Suma, K. J Pacing Clin Electrophysiol (2001) 24:1; 88- 96
Image of Dr. Tawara in the public domain after copyright expiration in 1970.
- Details
- Written by: Efrain A. Miranda, Ph.D.
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.
Giovanni Paolo Mascagni (1755-1815). Italian physician and anatomist whose meticulous research and illustrations revolutionized the understanding of the lymphatic system. Born in the mid-18th century, Mascagni's career spanned teaching, research, and political turbulence, culminating in posthumous publications that solidified his legacy. However, his work was marred by a posthumous scandal involving theft and plagiarism by his former assistant, Francesco Antommarchi.
Paolo Mascagni was born on January 25, 1755, in Pomarance (near Volterra), Italy, to Aurelio Mascagni and Elisabetta Burroni. Some accounts place his birthplace in the nearby village of Castelleto. He received his early education at home, focusing on philosophy, literature, physics, and mathematics, before enrolling at the University of Siena to study medicine. Mascagni graduated with a medical degree in 1777. He was appointed assistant prosector to the anatomist Pietro Tabarrani (1702 - 1779). Following Tabarrani's death, he succeeded him as anatomy lecturer at the University of Siena.
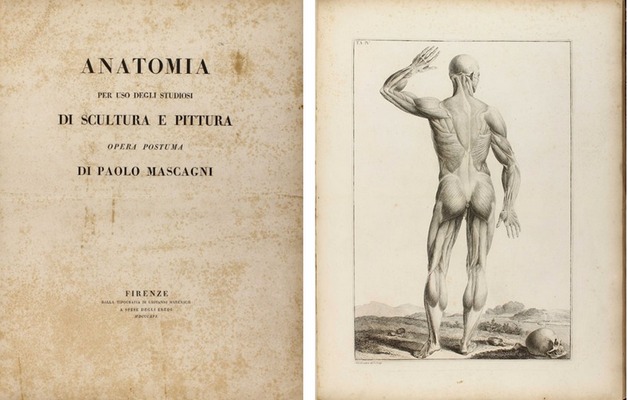
Mascagni's career was marked by academic accolades and political challenges. In 1796, he was elected a corresponding member of the Royal Swedish Academy of Sciences, and in 1798, he became president of the “Accademia dei Fisiocritici”(see end notes) in Siena. His Jacobin sympathies during the French occupation of Tuscany in 1799 led to his appointment as superintendent of arts, sciences, and charitable institutions, but after the French were expelled, he faced arrest and seven months in prison. Freed by royal decree in 1801, Mascagni was appointed professor of anatomy at the University of Pisa and a lecturer at the Hospital of Santa Maria Nuova in Florence. By 1807, he held the chair of anatomy at the University of Florence, where he also taught anatomy to artists, painters, and sculptors. As a result of his interest in human anatomy and art, the book “Anatomia per uso degli studiosi di scultura e pittura. Opera postuma” (Anatomy for the use of students of sculpture and painting) was published in 1816, one year after his death.
An accomplished artist himself, Mascagni collaborated with sculptor Clemente Susini (1754 – 1814) to create approximately 800 anatomical wax models, some of which are preserved in European museums: Museo La Specola, Florence, Italy; Museum Josephinum, Viena, Austria, etc. He also mentored Sardinian anatomist Francesco Antonio Boi (1767 – 1850), contributing to wax models now held in the Museo Archeologico Nazionale in Cagliari, Italy.
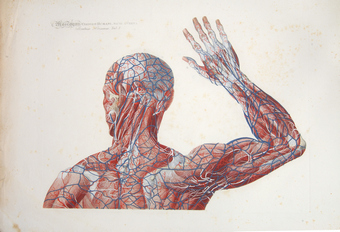
Mascagni's innovative techniques, such as injecting mercury into lymphatic vessels for visualization, allowed him to map a large part of the human lymphatic system, disproving earlier theories and highlighting its role in absorption and pathology. He is also credited with the early discovery of meningeal lymphatic vessels, later confirmed in modern studies (2014–2017). Mascagni died of sepsis on October 19, 1815, in Chiusdino, Italy.
Mascagni's publications blend scientific precision with artistic illustration. His 1784 work,” Prodrome d'un ouvrage sur le systeme des vaisseaux lymphatiques” (Initial notes on a work on the system of the lymphatic vessels), detailed his research on the lymphatic vessels and earned a prize from the Paris Academy of Sciences. This was followed by his 1787 publication “Vasorum lymphaticorum corporis humani historia et iconographia” (History and images of the lymphatic vessels of the human body), featuring 41 copperplates that provided the first complete description of the lymphatic system.
His most famous work was published after his death. He wanted to be able to depict the human anatomy in layers on a 5.9 ft. full-size person. Since this was not possible (see end notes), he worked with the artist and engraver Antonio Serantoni (1780 – 1837) to prepare three images of each plate in what is today known as the largest anatomy book ever published. Each page was printed in what is known as “double elephant folio”. To draw each plate, he dissected human bodies with the help of his assistant François (Francesco) Carlo Antommarchi (1780 – 1838).
After his death, with the help of family members and three professors on the Faculty at Pisa University (see end notes), his magnum opus “Icones Anatomiae Universae” (Images of Universal Anatomy”, was released in nine fascicles from 1823 to 1832, comprising 44 hand-colored copperplates and duplicates of each image (44 additional white and black pages) with symbols to identify each anatomical structure. The images depicted life-size layered views of the human body, from muscles to skeleton. These plates, engraved by Serantoni and others, covered the skeleton, viscera, cardiovascular and nervous systems, and more.
Because of the size, and the need to hand-color each of the 44 plates, and the publishing in fascicles, not many of these books were printed. The total number of the prints is unknown. What we do know is that today there are only 16 surviving complete copies of this incredible book, one of which can be seen at the Henry R. Winkler Center for the History of the Health Professions at the University of Cincinnati Medical College.
Following Mascagni's death, a scandal erupted involving his former prosector, Francesco Antommarchi. He took three sets of Mascagni's anatomical plates with him to St. Helena in 1815, where he served as Napoleon's physician. Upon Napoleon's death he stole Napoleon's death mask and passed it as his, attempting to make copies for sale. Defying a court ruling, Antommarchi published an unauthorized edition of Mascagni's book in Paris between 1823 and 1826. This version used 45 lithographed plates, omitting 24 figures from Mascagni's original and featuring inferior quality compared to the copper engravings. The theft and plagiarism by Antommarchi marred Mascagni’s vision. Only 8 of these books we published, one is lost, 6 are in private hands and the last one is in a library in Colombia.
Dr. Miranda during his presentation at the
XLIII Anatomy Meeting in Chile
Personal note: Research on Paolo Mascagni has been important for me in the search for larger anatomical images. With the help of the University of Cincinnati Daniel Harrison Medical Library, I was able to use scans of Mascagni’s book and digitally join the images to present them as Mascagni intended. These full-size images are now part of my library and the library of my good friend Dr. Randall K. Wolf. The full-size image can also be seen at the Anatomy Learning Lab of the University of Cincinnati.
In 2023 I was invited to lecture on this topic at the Vesalius Triennial AEIMS, Antwerp – Belgium, and the same year at the XLIII Congreso Chileno de Anatomía.
End notes:
1. The “Accademia dei Fisiocritici” was founded in 1691 and is the second oldest scientific society in the world, second only to the “Fellowship of the Royal Society” of London, England, founded in 1660.
2. Andrea Vaccá-Berlinghieri (1772-1826) Professor of Surgery, Giacomo Barzellotti (1768-1839) Professor of Surgery, Giovanni Rosini (1776-1855) Professor of Eloquence. The publisher was Nicolaum Capurro.
Sources
1. “Mascagni. Paolo” Stefano Arieti. Dizionario Biografico degli Italiani - Volume 71 (2008)
2. "Art in science: Giovanni Paolo Mascagni and the art of anatomy". Di Matteo, N; Tarabella, V.; et al. Clin Orthop Relat Res. 2015 Mar;473(3):783-8.
3. "Books at Iowa: The Great Anatomy of Paolo Mascagni". Eimas, Richard
4. “The Anatomia Universa (1823) of Paolo Mascagni (1755–1815): The memory of a masterpiece in the history of anatomy after two centuries” Orsini, D; Saverino. D; Martini, M. Translational Research in Anatomy Vol 35, 2024, 100285 https://doi.org/10.1016/j.tria.2024.100285.
5. “The “prince of anatomists” Paolo Mascagni and the modernity of his approach to teaching through the anatomical tables of his Anatomia universa. A pioneer and innovator in medical education at the end of the 18th century and the creator of unique anatomica” Martini, M; Orsini, D. Italian Journal of Anatomy and Embryology.
6. “Una autobiografia inedita di Paolo Mascagni relativa specialmente al periodo delle rivoluzioni politiche avvenute in Toscana alla fine del sec. XVIII ed alle persecuzioni subite in tale epoca dal Mascagni stesso” Guerritore, T.G. 1928 Atti della Accademia dei Fisiocritici 10(3) 3-24
- Details
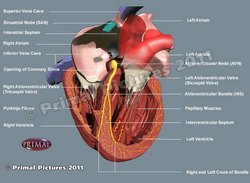
UPDATED: The sinoatrial node, is also known as the "sinuatrial node", "SA node" or by its eponym, the "node of Keith and Flack". It is the initial component of the conduction system of the heart.
It is a small nodule of cardiac muscle tissue, somewhat horseshoe-shaped that is found at the junction of the superior vena cava and the right atrium. Because of the inherent automaticity and rhythmical contractions of the SA node, it acts as the main pacemaker of the heart, being the base for normal heart beat, also known as "sinus rhythm"
It receives blood supply from the SA node artery, usually the first or second branch that arises off the right coronary artery. The SA node artery is a long vessel that passes between the right atrium and the ascending aorta on its way to the SA node.
The SA node receives innervation from both sympathetic and parasympathetic nerves. The parasympathetic innervation is by way of the vagus nerve, the Xth cranial nerve. The sympathetic innervation is by way of the cardiac nerves, a plexus that has its origin in the ventral rami of the first four thoracic spinal nerves (T1-T4).
The SA node was discovered in 1906 by Martin W. Flack (1882-1931) and Sir Arthur Keith (1866-1955). They named it originally the sino-auricular node.
Further studies by Cox (2020) have demonstrated that the SA node is not a single area of the right atrium, but rather expansive areas that beat at different beats per minute depending on the cardiac demand.
“Cardiac anatomy pertinent to the catheter and surgical treatment of atrial fibrillation”. Cox. JL et al J Cardiovasc Electrophysiol 2020 Aug;31(8):2118-2127. doi: 10.1111/jce.14440.
Click on the image for a larger version. Image modified from the original: "3D Human Anatomy: Regional Edition DVD-ROM." Courtesy of Primal Pictures
- Details
- Written by: Efrain A. Miranda, Ph.D.
The term “Bachmann’s bundle” refers to an eponymic structure associated with Jean George Bachmann (1877-1959) a French physician and physiologist. The proper anatomical term for this structure is “interatrial bundle” (Lat. fasciculus interatrialis).
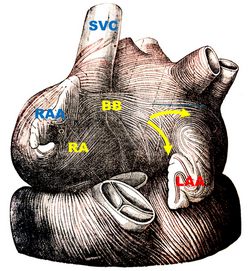
In 1916 Bachmann published a paper titled “The Inter-Auricular Time Interval” in the American Journal of Physiology. He measured activation times between the right and left atria and demonstrated that interruption of this distinct anterior interatrial muscular band resulted in delayed left atrial activation. He concluded that this band constituted the principal route for rapid interatrial conduction. The image, from his original publication, shows a dog’s heart with Bachmann’s bundle.
Bachmann’s bundle is a broad, flat band of atrial myocardium that crosses the superior aspect of the interatrial sulcus. It extends from the right atrium close to the junction of the right atrial appendage and the superior vena cava, and courses leftward across the interatrial groove to insert into the base of the left atrial appendage and the anterosuperior left atrial wall. The bundle is well-delineated and in most cases, a fine fatty layer is interposed between the underlying myocardium and the bundle.
This bundle contains predominantly longitudinally oriented myocardial fibers, aiding in fast passage of the electrical depolarization from the right atrium to the left atrium. This explains why, under normal conditions, the left atrium contracts only milliseconds after the right atrium. Bachmann's bundle is one of the components of the cardiac conduction system, and forms part of the specialized bundles of myocardial tissue that take the electrical impulses from the sinoatrial node to the atrioventricular node and the left atrium,
When Bachmann’s bundle is intact, left atrial activation is almost simultaneous with the right atrium. If it is damaged, it can cause varying degrees of interatrial block (IAB), and electrical conduction must proceed through other less effective pathways, resulting in atrial dyssynchrony and altered cardiac rhythm. Advanced IAB is strongly associated with atrial fibrillation, left atrial mechanical dysfunction, and increased risk of stroke even in sinus rhythm.
IAB can be caused by fibrosis, fatty infiltration, atrial dilation, aging, ischemia, and iatrogenic damage in prior cardiac surgery or ablation. All these preferentially affect the anterosuperior interatrial region, explaining the bundle’s vulnerability.
There are anatomical variations of Bachmann's bundle. In some cases, the bundle is separated from the atrial wall by epicardial fat, and in some cases it hugs the surface of the atria. In this last instance the bundle is more susceptible to damage by internal ablation in the left atrial wall. The location of the bundle can also vary.
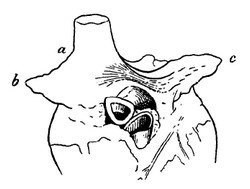
Bachmann’s bundle shows some bifurcations, helping to distribute the depolarization to the left atrium. The image, from Testut & Latarjet (1931), shows one of these bifurcations (yellow arrows). The bundle splits around the base of the left atrial appendage (LAA).
Historically, all pacemakers terminal wires have been implanted in the right atrium. but the potential dysfunction of Bachmann's bundle would require biatrial pacing, which is not used today.
Sources and references
1. Bachmann G. “The inter-auricular time interval”. Am J Physiol. 1916;41:309–320.
2. Hurst JW. “Profiles in Cardiology: Jean George Bachmann (1877–1959)”. Clin Cardiol. 1987;10:185–187.
3. Lemery R, Guiraudon G, Veinot JP. “Anatomic description of Bachmann’s bundle and its relation to the atrial septum”. Am J Cardiol. 2003;91:148–152.
4. Antonio Bayés de Luna, Albert Massó-van Roessel, Luis Alberto Escobar Robledo, The Diagnosis and Clinical Implications of Interatrial Block, European Cardiology Review 2015;10(1):54–9
5. Knol WG, de Vos CB, Crijns HJGM, et al. “The Bachmann bundle and interatrial conduction” Heart Rhythm. 2019;16:127–133.
6. “Iatrogenic biatrial flutter. The role of the Bachmann’s bundle” Constán E.; García F., Linde, A.. Complejo Hospitalario de Jaén, Jaén. Spain
7. "Tratado de Anatomia Humana" Testut et Latarjet 8th Ed. 1931 Salvat Editores, Spain
8. 4. Rigamonti F, Shah DC. "Bachmann Bundle Block Occurring During Radiofrequency Ablation at the Inter-Atrial Septum" J Clin Med. 2012;15(9):263.
9. Zhang Y, Wu F, Gao Y, Wu N, Yang G, Li M, Zhou L, Xu D, Chen M. "Bachmann bundle impairment following linear ablation of left anterior wall: impact on left atrial function". Int J Cardiovasc Imaging. 2022 Jan;38(1):41-50
10. Platonov, PG; Mitrofanova, L, et al.Substrates for intra-atrial and interatrial conduction in the atrial septum: Anatomical study on 84 human hearts Heart Rhythm,(2008)5:8,1189-1195.
- Details
- Written by: Efrain A. Miranda, Ph.D.
This article is part of the series "A Moment in History" where we honor those who have contributed to the growth of medical knowledge in the areas of anatomy, medicine, surgery, and medical research.
Jean George Bachmann (1877–1959) was a French physician–physiologist whose experimental work in the early twentieth century provided the first clear functional description of a preferential interatrial conduction pathway. This structure, eponymically named “Bachmann’s bundle”, plays a central role in normal atrial activation and in the pathophysiology of interatrial block and atrial arrhythmias.
As a young man, Bachmann served as a merchant sailor, crossing the Atlantic multiple times. He emigrated to the United States in 1902 and earned his medical degree at the top of his class from Jefferson Medical College in Philadelphia in 1907. He stayed at this Medical College as a demonstrator and physiologist. In 1910, he joined Emory University in Atlanta. Between 1917 -1918 he served as a medical officer in the US Army. He retired from Emory in 1947 and continued his private medical practice until his death in 1959.
On the personal side, Bachmann was a man of many talents: a polyglot, he was fluent in German, French, Spanish and English. He was a chef in his own right and occasionally worked as a chef in international hotels. In fact, he paid his tuition at Jefferson Medical College, working both as a chef and as a language tutor.
The intrinsic cardiac conduction system was a major focus of cardiovascular research in the late nineteenth and early twentieth centuries. The atrioventricular (AV) node was discovered and described by Sunao Tawara and Karl Albert Aschoff in 1906, and the sinoatrial node by Sir Arthur Keith and Martin W. Flack in 1907.
While the connections that distribute the electrical impulse from the AV node to the ventricles were known through the works of Wilhelm His Jr, in 1893 and Jan Evangelista Purkinje in 1839, the mechanism by which electrical impulses spread between the atria remained uncertain.
In 1916 Bachmann published a paper titled “The Inter-Auricular Time Interval” in the American Journal of Physiology. Bachmann measured activation times between the right and left atria and demonstrated that interruption of a distinct anterior interatrial muscular band resulted in delayed left atrial activation. He concluded that this band constituted the principal route for rapid interatrial conduction.
Subsequent anatomical and electrophysiological studies confirmed the importance of the structure described by Bachmann, which came to bear his name. Bachmann’s bundle is now recognized as a key determinant of atrial activation patterns, and its dysfunction is associated with interatrial block, atrial fibrillation, and abnormal P-wave morphology. His work remains foundational in both basic cardiac anatomy and clinical electrophysiology.
Sources and references
1. Bachmann G. “The inter-auricular time interval”. Am J Physiol. 1916;41:309–320.
2. Hurst JW. “Profiles in Cardiology: Jean George Bachmann (1877–1959)”. Clin Cardiol. 1987;10:185–187.
3. Lemery R, Guiraudon G, Veinot JP. “Anatomic description of Bachmann’s bundle and its relation to the atrial septum”. Am J Cardiol. 2003;91:148–152.
4. "Remembering the canonical discoverers of the core components of the mammalian cardiac conduction system: Keith and Flack, Aschoff and Tawara, His, and Purkinje" Icilio Cavero and Henry Holzgrefe Advances in Physiology Education 2022 46:4, 549-579.
5. Knol WG, de Vos CB, Crijns HJGM, et al. “The Bachmann bundle and interatrial conduction” Heart Rhythm. 2019;16:127–133.
6. “Iatrogenic biatrial flutter. The role of the Bachmann’s bundle” Constán E.; García F., Linde, A.. Complejo Hospitalario de Jaén, Jaén. Spain
7. Keith A, Flack M. The form and nature of the muscular connections between the primary divisions of the vertebrate heart. J Anat Physiol 41: 172–189, 1907.
- Details
- Written by: Efrain A. Miranda, Ph.D.

Homeostasis is the coordinated set of physiological mechanisms that preserve a stable internal bodily environment (through feedback-controlled regulatory processes) despite fluctuations in the external environment. The concept applies to many dynamic regulations of physiological variables such as body temperature, pH, electrolyte balance, osmolarity, blood glucose, etc.
Claude Bernard (1813–1878) introduced the concept of a “milieu intérieur” the “internal environment” in 1865 where he stated “La fixité du milieu intérieur est la condition de la vie libre et indépendante.” (The constancy of the internal environment is the condition for a free and independent life). Walter B. Cannon (1871–1945) formally coined the term homeostasis in 1929. In his reasoning to name these processes under one name he used the Greek term "ομοιόσταση" [omeóstasí) meaning "constant & stable" or "similar & standing still" referring to a constant (internal) environment.
Disruption of homeostatic processes can contribute to disease states such as diabetes mellitus (failure of glucose homeostasis), heart failure (impaired circulatory stability), heat stroke and/or hypothermia (thermoregulatory failure), hyponatremia or hypernatremia (electrolyte imbalance), etc.
For additional information here is an article from the National Library of Medicine.
Sources:
1. Claude Bernard, "Introduction à l’étude de la médecine expérimentale" (1865).
2. “Organization for physiological homeostasis” Cannon W. B.; Physiol Rev. 1929; 9:399–431.
3. "Textbook of Medical Physiology"; Guyton, Arthur C and Hall, John E ISBN: 0721659446 USA: W.B. Saunders, 1996.
4. “Homeostasis and Body Fluid Regulation: An End Note”. De Luca LA Jr, David RB, Menani JV. Neurobiology of Body Fluid Homeostasis: Transduction and Integration. Boca Raton (FL): CRC Press/Taylor & Francis; 2014. Chapter 15